Fluid accumulation in the tissue and air spaces of the lungs
Medical condition
| Pulmonary edema
|
|---|
| Other names
| Pulmonary oedema
|
|---|
 |
| Pulmonary edema with small
pleural effusions
on both sides
|
| Specialty
| Cardiology
,
critical care medicine
pulmonology
|
|---|
| Symptoms
| Progressive dyspnea, cough, fever, cyanosis, tachycardia
|
|---|
| Complications
| ARDS, respiratory failure
|
|---|
| Causes
| Cardiogenic, Noncardiogenic (pneumonia, inhalation injury, sepsis, airway obstruction, high altitude)
|
|---|
| Diagnostic method
| Medical imaging, lab tests, ECG, echocardiography
|
|---|
| Treatment
| Supplemental oxygen, diuretics, treat underlying disease process
|
|---|
Pulmonary edema
(
British English
: oedema), also known as
pulmonary congestion
, is excessive
fluid accumulation
in the
tissue
or
air spaces
(usually
alveoli
) of the
lungs
.
[1]
This leads to impaired
gas exchange
, most often leading to
dyspnea
which can progress to
hypoxemia
and
respiratory failure
. Pulmonary edema has multiple causes and is traditionally classified as
cardiogenic
(caused by the heart) or noncardiogenic (all other types not caused by the heart).
[2]
[3]
Various laboratory tests (
CBC
,
troponin
,
BNP
, etc.) and imaging studies (
chest x-ray
,
CT scan
,
ultrasound
) are often used to diagnose and classify the cause of pulmonary edema.
[4]
[5]
[6]
Treatment is focused on three aspects: improving respiratory function, treating the underlying cause, and preventing further damage and allow full recovery to the lung. Pulmonary edema can cause permanent organ damage, and when sudden (acute), can lead to
respiratory failure
or
cardiac arrest
due to
hypoxia
.
[7]
The term edema is from the
Greek
ο?δημα
(
oid?ma
, "swelling"), from ο?δ?ω (
oide?
, "(I) swell").
[8]
[9]
Pathophysiology
[
edit
]
The amount of fluid in the lungs is governed by multiple forces and is visualized using the
Starling equation
. There are two
hydrostatic pressures
and two
oncotic (protein) pressures
that determine the fluid movement within the lung air spaces (
alveoli
). Of the forces that explain fluid movement, only the
pulmonary wedge pressure
is obtainable via
pulmonary artery catheterization
.
[10]
Due to the complication rate associated with pulmonary artery catheterization, other imaging modalities and diagnostic methods have become more popular.
[11]
Imbalance in any of these forces can cause fluid movement (or lack of movement) causing a buildup of fluid where it should not normally be. Although rarely clinically measured, these forces allow physicians to classify and subsequently treat the underlying cause of pulmonary edema.
Classification
[
edit
]
Pulmonary edema has a multitude of causes, and is typically classified as cardiogenic or noncardiogenic. Cardiogenic pulmonary edema is caused by increased hydrostatic pressure causing increased fluid in the pulmonary interstitium and
alveoli
. Noncardiogenic causes are associated with the oncotic pressure as discussed above causing malfunctioning barriers in the lungs (increased
microvascular permeability
).
[12]
Cardiogenic
[
edit
]
Cardiogenic pulmonary edema is typically caused by either volume overload or impaired
left ventricular
function. As a result,
pulmonary pressures
rises from the normal average of 15 mmHg.
[13]
As the pulmonary pressure rises, these pressures overwhelm the barriers and fluid enters the alveoli when the pressure is above 25 mmHg.
[14]
Depending whether the cause is acute or chronic determines how fast pulmonary edema develops and the severity of symptoms.
[12]
Some of the common causes of cardiogenic pulmonary edema include:
- Acute exacerbation of
congestive heart failure
which is due to the heart's inability to pump the blood out of the pulmonary circulation at a sufficient rate resulting in elevation in
pulmonary wedge pressure
and edema.
- Pericardial tamponade
as well as treating pericardial tamponade via
pericardiocentesis
has shown to cause pulmonary edema as a result of increased left-sided heart strain.
[15]
- Heart Valve Dysfunction
such as mitral valve regurgitation can cause increased pressure and energy on the left side of the heart (increased pulmonary wedge pressure) causing pulmonary edema.
[16]
- Hypertensive crisis
can cause pulmonary edema as the elevation in blood pressure and increased
afterload
on the left ventricle hinders forward flow in blood vessels and causes the elevation in
wedge pressure
and subsequent pulmonary edema. In a recent systematic review, it was found that pulmonary edema was the second most common condition associated with hypertensive crisis after
ischemic stroke
.
[17]
Flash Pulmonary Edema
[
edit
]
A particularly severe type of cardiogenic pulmonary edema is flash pulmonary edema (FPE). Flash pulmonary edema is a clinical syndrome of acute heart failure that begins suddenly and accelerates rapidly. Frequently the most noticeable abnormality is edema of the lungs. Nevertheless it is a cardiovascular disease not a pulmonary disease. It is also known by other appellations including sympathetic crashing acute pulmonary edema (SCAPE).
[18]
It is often associated with severe hypertension
[19]
Typically, patients with the syndrome of flash pulmonary edema do not have chest pain are often not recognized as having a cardiovascular disease. Treatment of FPE should include reducing systemic vascular resistance with nitroglycerin, providing supplemental oxygenation, and decreasing pulmonary circulation pressures while FPE stays.
[20]
Recurrence of FPE is thought to be associated with
hypertension
[21]
and may signify
renal artery stenosis
.
[22]
Prevention of recurrence is based on managing or preventing hypertension,
coronary artery disease
,
renovascular hypertension
, and heart failure.
Noncardiogenic
[
edit
]
Noncardiogenic pulmonary edema is caused by increased
microvascular permeability
(increased
oncotic pressure
) leading to increased fluid transfer into the alveolar spaces. The pulmonary artery wedge pressure is typically normal as opposed to cardiogenic pulmonary edema where the elevated pressure is causing the fluid transfer. There are multiple causes of noncardiogenic edema with multiple subtypes within each cause.
Acute respiratory distress syndrome
(ARDS) is a type of respiratory failure characterized by rapid onset of widespread inflammation in the lungs. Although ARDS can present with pulmonary edema (fluid accumulation), it is a distinct clinical syndrome that is not synonymous with pulmonary edema.
Direct Lung Injury
[
edit
]
Acute lung injury
may cause pulmonary edema directly through injury to the vasculature and parenchyma of the lung, causes include:
- Inhalation of hot or toxic gases
[12]
(including
vaping-associated lung injury
)
- Pulmonary contusion
, i.e.,
high-energy trauma
(e.g. vehicle accidents)
- Aspiration
, e.g., gastric fluid
- Reexpansion, i.e. post large volume
thoracocentesis
, resolution of pneumothorax, post decortication, removal of endobronchial obstruction, effectively a form of negative pressure pulmonary oedema.
- Reperfusion injury, i.e., postpulmonary
thromboendartectomy
or
lung transplantation
- Swimming induced pulmonary edema
also known as immersion pulmonary edema
[23]
[24]
[25]
- Transfusion associated Acute Lung Injury
is a specific type of blood-product transfusion injury that occurs when the donors plasma contained antibodies against the recipient, such as anti-HLA or anti-neutrophil antibodies.
[26]
Indirect Lung Injury
[
edit
]
Special Causes
[
edit
]
Some causes of pulmonary edema are less well characterized and arguably represent specific instances of the broader classifications above.
Signs and symptoms
[
edit
]
 Fluid within the
alveoli
(air spaces) of the
lungs
Fluid within the
alveoli
(air spaces) of the
lungs
The most common symptom of pulmonary edema is
dyspnea
and may include other symptoms relating to inadequate oxygen (
hypoxia
) such as fast breathing (
tachypnea
),
tachycardia
and
cyanosis
. Other common symptoms include
coughing up blood
(classically seen as pink or red, frothy sputum),
excessive sweating
,
anxiety
, and
pale skin
. Other signs include end-inspiratory
crackles
(crackling sounds heard at the end of a deep breath) on
auscultation
and the presence of a
third heart sound
.
[3]
Shortness of breath
can manifest as
orthopnea
(inability to breathe sufficiently when lying down flat due to breathlessness) and/or
paroxysmal nocturnal dyspnea
(episodes of severe sudden breathlessness at night). These are common presenting symptoms of chronic and cardiogenic pulmonary edema due to left ventricular failure.
The development of pulmonary edema may be associated with symptoms and signs of "fluid overload" in the lungs; this is a non-specific term to describe the manifestations of
right
ventricular failure on the rest of the body. These symptoms may include peripheral
edema
(swelling of the legs, in general, of the "pitting" variety, wherein the skin is slow to return to normal when pressed upon due to fluid), raised
jugular venous pressure
and
hepatomegaly
, where the liver is excessively enlarged and may be tender or even pulsatile.
Additional symptoms such as fever, low blood pressure, injuries or burns may be present and can help characterize the cause and subsequent treatment strategies.
Diagnosis
[
edit
]
 Chest X-ray
of Pulmonary Edema with lines and overlay showing congestion
Chest X-ray
of Pulmonary Edema with lines and overlay showing congestion
There is no single test for confirming that breathlessness is caused by pulmonary edema ? there are many causes of
shortness of breath
; but there are methods to suggest a high probability of an edema.
Lab Tests
[
edit
]
Low
oxygen saturation
in blood and disturbed
arterial blood gas
readings support the proposed diagnosis by suggesting a
pulmonary shunt
. Blood tests are performed for
electrolytes
(sodium, potassium) and markers of
renal function
(creatinine, urea). Elevated creatine levels may suggest a cardiogenic cause of pulmonary edema.
[12]
Liver enzymes
, inflammatory markers (usually
C-reactive protein
) and a
complete blood count
as well as
coagulation
studies (PT, aPTT) are also typically requested as further diagnosis. Elevated white blood cell count (
WBC
) may suggest a non-cardiogenic cause such as sepsis or infection.
[12]
B-type natriuretic peptide
(BNP) is available in many hospitals, sometimes even as a point-of-care test. Low levels of BNP (<100 pg/ml) suggest a cardiac cause is unlikely, and suggest noncardiogenic pulmonary edema.
[3]
Imaging Tests
[
edit
]
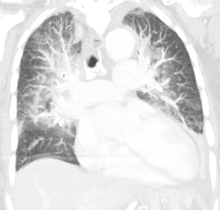 Pulmonary edema on CT-scan (coronal
MPR
)
Pulmonary edema on CT-scan (coronal
MPR
)
Chest X-ray has been used for many years to diagnose pulmonary edema due to its wide availability and relatively cheap cost.
[4]
A
chest X-ray
will show fluid in the alveolar walls,
Kerley B lines
, increased vascular shadowing in a classical batwing peri-
hilum
pattern, upper lobe diversion (biased blood flow to the superior parts instead of inferior parts of the lung), and possibly
pleural effusions
. In contrast, patchy alveolar infiltrates are more typically associated with noncardiogenic edema.
[3]
Lung
ultrasounds
, employed by a healthcare provider at the point of care, is also a useful tool to diagnose pulmonary edema; not only is it accurate, but it may quantify the degree of lung water, track changes over time, and differentiate between cardiogenic and non-cardiogenic edema.
[36]
Lung ultrasound is recommended as the first-line method due to its wide availability, ability to be performed bedside, and wide diagnostic utility for other similar diseases.
[4]
Especially in the case of cardiogenic pulmonary edema, urgent
echocardiography
may strengthen the diagnosis by demonstrating impaired left ventricular function, high
central venous pressures
and high
pulmonary artery
pressures leading to pulmonary edema.
Prevention
[
edit
]
In those with underlying heart or lung disease, effective control of congestive and respiratory symptoms can help prevent pulmonary edema.
[37]
Dexamethasone
is in widespread use for the prevention of
high altitude pulmonary edema
.
Sildenafil
is used as a preventive treatment for altitude-induced pulmonary edema and pulmonary hypertension.
[38]
[39]
Sildenafil's mechanism of action is via phosphodiesterase inhibition which raises cGMP, resulting in pulmonary arterial vasodilation and inhibition of smooth muscle cell proliferation and indirectly fluid formation in the lungs.
[40]
While this effect has only recently been discovered, sildenafil is already becoming an accepted treatment for this condition, in particular in situations where the standard treatment of rapid descent (acclimatization) has been delayed for some reason.
[41]
Management
[
edit
]
The initial management of pulmonary edema, irrespective of the type or cause, is supporting vital functions while edema lasts.
Hypoxia
may require supplementary oxygen to balance blood oxygen levels, but if this is insufficient then again mechanical ventilation may be required to prevent complications caused by hypoxia.
[42]
Therefore, if the level of consciousness is decreased it may be required to proceed to
tracheal intubation
and
mechanical ventilation
to prevent airway compromise. Treatment of the underlying cause is the next priority; pulmonary edema secondary to infection, for instance, would require the administration of appropriate
antibiotics
or
antivirals
.
[2]
[3]
Cardiogenic pulmonary edema
[
edit
]
Acute cardiogenic pulmonary edema often responds rapidly to medical treatment.
[43]
Positioning upright may relieve symptoms. A
loop diuretic
such as
furosemide
is administered, often together with
morphine
to reduce respiratory distress.
[43]
Both diuretic and morphine may have
vasodilator
effects, but specific vasodilators may be used (particularly intravenous
glyceryl trinitrate
or
ISDN
) provided the blood pressure is adequate.
[43]
Continuous positive airway pressure
and
bilevel positive airway pressure
(CPAP/BiPAP) has been demonstrated to reduce mortality and the need of mechanical ventilation in people with severe cardiogenic pulmonary edema.
[44]
It is possible for cardiogenic pulmonary edema to occur together with
cardiogenic shock
, in which the cardiac output is insufficient to sustain an adequate blood pressure to the lungs. This can be treated with
inotropic agents
or by
intra-aortic balloon pump
, but this is regarded as temporary treatment while the underlying cause is addressed and the lungs recover.
[43]
Prognosis
[
edit
]
As pulmonary edema has a wide variety of causes and presentations, the outcome or prognosis is often disease-dependent and more accurately described in relation to the associated syndrome. It is a major health problem, with one large review stating an incidence of 7.6% with an associated in hospital mortality rate of 11.9%.
[2]
Generally, pulmonary edema is associated with a poor prognosis with a 50% survival rate at one year, and 85% mortality at six years.
[45]
References
[
edit
]
- ^
Dorland's illustrated medical dictionary
(32nd ed.). Saunders/Elsevier. 2 May 2011. p. 593.
ISBN
978-1-4160-6257-8
.
- ^
a
b
c
Assaad S, Kratzert WB, Shelley B, Friedman MB, Perrino A (April 2018).
"Assessment of Pulmonary Edema: Principles and Practice"
(PDF)
.
Journal of Cardiothoracic and Vascular Anesthesia
.
32
(2): 901?914.
doi
:
10.1053/j.jvca.2017.08.028
.
PMID
29174750
.
- ^
a
b
c
d
e
Ware LB, Matthay MA (December 2005). "Clinical practice. Acute pulmonary edema".
The New England Journal of Medicine
.
353
(26): 2788?2796.
doi
:
10.1056/NEJMcp052699
.
PMID
16382065
.
- ^
a
b
c
Lindow T, Quadrelli S, Ugander M (November 2023).
"Noninvasive Imaging Methods for Quantification of Pulmonary Edema and Congestion: A Systematic Review"
.
JACC. Cardiovascular Imaging
.
16
(11): 1469?1484.
doi
:
10.1016/j.jcmg.2023.06.023
.
PMID
37632500
.
- ^
Guo L, Yang X, Yang B, Tang G, Li C (July 2023).
"Prevalence, in-hospital mortality, and factors related to neurogenic pulmonary edema after spontaneous subarachnoid hemorrhage: a systematic review and meta-analysis"
.
Neurosurgical Review
.
46
(1): 169.
doi
:
10.1007/s10143-023-02081-6
.
PMC
10335949
.
PMID
37432487
.
- ^
Komiya K, Akaba T, Kozaki Y, Kadota JI, Rubin BK (August 2017).
"A systematic review of diagnostic methods to differentiate acute lung injury/acute respiratory distress syndrome from cardiogenic pulmonary edema"
.
Critical Care
.
21
(1): 228.
doi
:
10.1186/s13054-017-1809-8
.
PMC
6389074
.
PMID
28841896
.
- ^
Siddiqi TJ, Usman MS, Rashid AM, Javaid SS, Ahmed A, Clark D, et al. (July 2023).
"Clinical Outcomes in Hypertensive Emergency: A Systematic Review and Meta-Analysis"
.
Journal of the American Heart Association
.
12
(14): e029355.
doi
:
10.1161/JAHA.122.029355
.
PMC
10382109
.
PMID
37421281
.
- ^
ο?δημα
,
ο?δ?ω
.
Liddell, Henry George
;
Scott, Robert
;
A Greek?English Lexicon
at the
Perseus Project
.
- ^
Harper D.
"edema"
.
Online Etymology Dictionary
.
- ^
Patel MR, Bailey SR, Bonow RO, Chambers CE, Chan PS, Dehmer GJ, et al. (May 2012).
"ACCF/SCAI/AATS/AHA/ASE/ASNC/HFSA/HRS/SCCM/SCCT/SCMR/STS 2012 appropriate use criteria for diagnostic catheterization: a report of the American College of Cardiology Foundation Appropriate Use Criteria Task Force, Society for Cardiovascular Angiography and Interventions, American Association for Thoracic Surgery, American Heart Association, American Society of Echocardiography, American Society of Nuclear Cardiology, Heart Failure Society of America, Heart Rhythm Society, Society of Critical Care Medicine, Society of Cardiovascular Computed Tomography, Society for Cardiovascular Magnetic Resonance, and Society of Thoracic Surgeons"
.
Journal of the American College of Cardiology
.
59
(22): 1995?2027.
doi
:
10.1016/j.jacc.2012.03.003
.
PMID
22578925
.
- ^
Rajaram SS, Desai NK, Kalra A, Gajera M, Cavanaugh SK, Brampton W, et al. (February 2013).
"Pulmonary artery catheters for adult patients in intensive care"
.
The Cochrane Database of Systematic Reviews
.
2013
(2) CD003408: CD003408.
doi
:
10.1002/14651858.CD003408.pub3
.
PMC
6517063
.
PMID
23450539
.
- ^
a
b
c
d
e
Vincent J, Moore FA, Bellomo R, Marini JJ, eds. (2024).
Textbook of critical care
(8th ed.). Amsterdam: Elsevier.
ISBN
978-0-323-75929-8
.
- ^
What Is Pulmonary Hypertension?
From Diseases and Conditions Index (DCI). National Heart, Lung, and Blood Institute. Last updated September 2008. Retrieved on 6 April 2009.
- ^
Adair OV (2001).
Cardiology secrets
(2nd ed.). Elsevier Health Sciences. Chapter 41, page 210.
ISBN
1-56053-420-6
.
- ^
Alerhand S, Adrian RJ, Long B, Avila J (August 2022). "Pericardial tamponade: A comprehensive emergency medicine and echocardiography review".
The American Journal of Emergency Medicine
.
58
: 159?174.
doi
:
10.1016/j.ajem.2022.05.001
.
PMID
35696801
.
S2CID
248620419
.
- ^
MacIver DH, Clark AL (April 2015). "The vital role of the right ventricle in the pathogenesis of acute pulmonary edema".
The American Journal of Cardiology
.
115
(7): 992?1000.
doi
:
10.1016/j.amjcard.2015.01.026
.
PMID
25697920
.
- ^
Siddiqi TJ, Usman MS, Rashid AM, Javaid SS, Ahmed A, Clark D, et al. (July 2023).
"Clinical Outcomes in Hypertensive Emergency: A Systematic Review and Meta-Analysis"
.
Journal of the American Heart Association
.
12
(14): e029355.
doi
:
10.1161/JAHA.122.029355
.
PMC
10382109
.
PMID
37421281
.
- ^
Siddiqua N, Mathew R, Sahu AK, Jamshed N, Bhaskararayuni J, Aggarwal P, et al. (January 2024). "High-dose versus low-dose intravenous nitroglycerine for sympathetic crashing acute pulmonary edema: a randomised controlled trial".
Emergency Medicine Journal
.
41
(2): 96?102.
doi
:
10.1136/emermed-2023-213285
.
PMID
38050078
.
S2CID
265507643
.
- ^
Gandhi SK, Powers JC, Nomeir AM, Fowle K, Kitzman DW, Rankin KM, Little WC (January 2001).
"The pathogenesis of acute pulmonary edema associated with hypertension"
.
The New England Journal of Medicine
.
344
(1): 17?22.
doi
:
10.1056/NEJM200101043440103
.
PMID
11136955
.
- ^
Long B, Koyfman A, Gottlieb M (November 2018). "Management of Heart Failure in the Emergency Department Setting: An Evidence-Based Review of the Literature".
The Journal of Emergency Medicine
.
55
(5): 635?646.
doi
:
10.1016/j.jemermed.2018.08.002
.
PMID
30266198
.
S2CID
52884356
.
- ^
Kramer K, Kirkman P, Kitzman D, Little WC (September 2000). "Flash pulmonary edema: association with hypertension and reoccurrence despite coronary revascularization".
American Heart Journal
.
140
(3): 451?455.
doi
:
10.1067/mhj.2000.108828
.
PMID
10966547
.
- ^
Pickering TG, Herman L, Devereux RB, Sotelo JE, James GD, Sos TA, et al. (September 1988). "Recurrent pulmonary oedema in hypertension due to bilateral renal artery stenosis: treatment by angioplasty or surgical revascularisation".
Lancet
.
2
(8610): 551?552.
doi
:
10.1016/S0140-6736(88)92668-2
.
PMID
2900930
.
S2CID
36141498
.
- ^
Hampson NB, Dunford RG (1997).
"Pulmonary edema of scuba divers"
.
Undersea & Hyperbaric Medicine
.
24
(1): 29?33.
PMID
9068153
. Archived from the original on 2010-06-17
. Retrieved
2008-09-04
.
{{
cite journal
}}
: CS1 maint: unfit URL (
link
)
- ^
Cochard G, Arvieux J, Lacour JM, Madouas G, Mongredien H, Arvieux CC (2005).
"Pulmonary edema in scuba divers: recurrence and fatal outcome"
.
Undersea & Hyperbaric Medicine
.
32
(1): 39?44.
PMID
15796313
. Archived from the original on September 20, 2008
. Retrieved
2008-09-04
.
{{
cite journal
}}
: CS1 maint: unfit URL (
link
)
- ^
Kumar M, Thompson PD (May 2019). "A literature review of immersion pulmonary edema".
The Physician and Sportsmedicine
.
47
(2): 148?151.
doi
:
10.1080/00913847.2018.1546104
.
PMID
30403902
.
S2CID
53209012
.
- ^
"Transfusion-related acute lung injury (TRALI)"
.
Professional Education
. 2016-06-17
. Retrieved
2016-12-03
.
- ^
Papaioannou V, Terzi I, Dragoumanis C, Pneumatikos I (2009). "Negative-pressure acute tracheobronchial hemorrhage and pulmonary edema".
Journal of Anesthesia
.
23
(3): 417?420.
doi
:
10.1007/s00540-009-0757-0
.
PMID
19685125
.
S2CID
9616605
.
- ^
Hines, Roberta L. and Marschall, Katherine. Stoelting's Anesthesia and Co-Existing Disease. 6th edition. 2012. pages 178 and 179.
- ^
"Pulmonary edema"
.
Mayo Clinic
. 2018-08-08.
- ^
O'Leary R, McKinlay J (2011).
"Neurogenic pulmonary oedema"
.
Continuing Education in Anaesthesia, Critical Care & Pain
.
11
(3): 87?92.
doi
:
10.1093/BJACEACCP/MKR006
.
S2CID
18066655
.
- ^
"Adverse Reactions"
.
Professional Education
. 2016-06-02. Archived from
the original
on 2016-12-20
. Retrieved
2016-12-03
.
- ^
Boyle AJ, Mac Sweeney R, McAuley DF (August 2013).
"Pharmacological treatments in ARDS; a state-of-the-art update"
.
BMC Medicine
.
11
: 166.
doi
:
10.1186/1741-7015-11-166
.
PMC
3765621
.
PMID
23957905
.
- ^
Luks AM (2008). "Do we have a "best practice" for treating high altitude pulmonary edema?".
High Altitude Medicine & Biology
.
9
(2): 111?114.
doi
:
10.1089/ham.2008.1017
.
PMID
18578641
.
- ^
Bates, M (2007).
"High altitude pulmonary edema"
. Altitude Physiology Expeditions
. Retrieved
2008-09-04
.
- ^
White J, Gray M, Fisher M (1989).
Atrax Robustus
IPCS InChem
- ^
Volpicelli G, Elbarbary M, Blaivas M, Lichtenstein DA, Mathis G, Kirkpatrick AW, et al. (April 2012).
"International evidence-based recommendations for point-of-care lung ultrasound"
.
Intensive Care Medicine
.
38
(4): 577?591.
doi
:
10.1007/s00134-012-2513-4
.
PMID
22392031
.
- ^
Light RW, Lee YC (2006-01-01). "PLEURAL EFFUSIONS | Overview". In Laurent GJ, Shapiro SD (eds.).
Encyclopedia of Respiratory Medicine
. Oxford: Academic Press. pp. 353?358.
doi
:
10.1016/b0-12-370879-6/00299-4
.
ISBN
978-0-12-370879-3
.
- ^
Richalet JP, Gratadour P, Robach P, Pham I, Dechaux M, Joncquiert-Latarjet A, et al. (February 2005).
"Sildenafil inhibits altitude-induced hypoxemia and pulmonary hypertension"
.
American Journal of Respiratory and Critical Care Medicine
.
171
(3): 275?281.
doi
:
10.1164/rccm.200406-804OC
.
PMID
15516532
.
- ^
Perimenis P (May 2005). "Sildenafil for the treatment of altitude-induced hypoxaemia".
Expert Opinion on Pharmacotherapy
.
6
(5): 835?837.
doi
:
10.1517/14656566.6.5.835
.
PMID
15934909
.
S2CID
24900169
.
- ^
Clark, Michael, Kumar, Parveen J. (2009).
Kumar and Clark's clinical medicine
. St. Louis, Mo: Elsevier Saunders. p. 783.
ISBN
978-0-7020-2993-6
.
- ^
Fagenholz PJ, Gutman JA, Murray AF, Harris NS (2007). "Treatment of high altitude pulmonary edema at 4240 m in Nepal".
High Altitude Medicine & Biology
.
8
(2): 139?146.
doi
:
10.1089/ham.2007.3055
.
PMID
17584008
.
- ^
MacIntyre NR (January 2013).
"Supporting oxygenation in acute respiratory failure"
.
Respiratory Care
.
58
(1): 142?150.
doi
:
10.4187/respcare.02087
.
PMID
23271824
.
- ^
a
b
c
d
Cleland JG, Yassin AS, Khadjooi K (February 2010).
"Acute heart failure: focusing on acute cardiogenic pulmonary oedema"
.
Clinical Medicine
.
10
(1): 59?64.
doi
:
10.7861/clinmedicine.10-1-59
.
PMC
4954483
.
PMID
20408310
.
- ^
Berbenetz N, Wang Y, Brown J, Godfrey C, Ahmad M, Vital FM, et al. (April 2019).
"Non-invasive positive pressure ventilation (CPAP or bilevel NPPV) for cardiogenic pulmonary oedema"
.
The Cochrane Database of Systematic Reviews
.
2019
(4): CD005351.
doi
:
10.1002/14651858.CD005351.pub4
.
PMC
6449889
.
PMID
30950507
.
- ^
Zanza C, Saglietti F, Tesauro M, Longhitano Y, Savioli G, Balzanelli MG, et al. (October 2023).
"Cardiogenic Pulmonary Edema in Emergency Medicine"
.
Advances in Respiratory Medicine
.
91
(5): 445?463.
doi
:
10.3390/arm91050034
.
PMC
10604083
.
PMID
37887077
.
| Classification
| |
|---|
| External resources
| |
|---|