Hyperkalemia is defined as a potassium level greater than 5.5 mEq/L.
[
1
]
It can be difficult to diagnose clinically because symptoms may be vague or absent. However, the fact that hyperkalemia can lead to sudden death from cardiac arrhythmias requires that physicians be quick to consider hyperkalemia in patients who are at risk for it.
[
2
,
3
]
Initial emergency department care includes assessment of the ABCs and prompt evaluation of the patient's cardiac status with an electrocardiogram (ECG). In patients in whom hyperkalemia is severe (potassium >7.0 mEq/L) or symptomatic, treatment should commence before diagnostic investigation of the underlying cause.
See the ECG below.
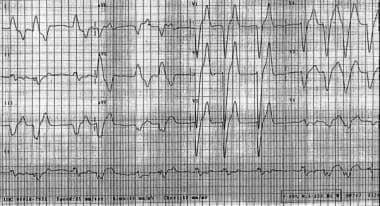 Widened QRS complexes in hyperkalemia.
Widened QRS complexes in hyperkalemia.
Signs and symptoms of hyperkalemia
Patients with hyperkalemia may be asymptomatic, or they may report the following symptoms (cardiac and neurologic symptoms predominate):
Evaluation of vital signs is essential for determining the patient’s hemodynamic stability and the presence of cardiac arrhythmias related to hyperkalemia.
[
1
]
Additional important components of the physical exam may include the following:
-
Cardiac examination may reveal extrasystoles, pauses, or bradycardia
-
Neurologic examination may reveal diminished deep tendon reflexes or decreased motor strength
-
In rare cases, muscular paralysis and hypoventilation may be observed
-
Signs of renal failure, such as edema, skin changes, and dialysis sites, may be present
-
Signs of trauma may indicate that the patient has rhabdomyolysis, which is one cause of hyperkalemia
See
Clinical Presentation
for more detail.
Diagnosis of hyperkalemia
Laboratory studies
The following lab studies can be used in the diagnosis of hyperkalemia:
-
Potassium level: The relationship between serum potassium level and symptoms is not consistent; for example, patients with a chronically elevated potassium level may be asymptomatic at much higher levels than other patients; the rapidity of change in the potassium level influences the symptoms observed at various potassium levels
-
Blood urea nitrogen (BUN) and creatinine levels: For evaluation of renal status
-
Calcium level: If the patient has renal failure (because hypocalcemia can exacerbate cardiac rhythm disturbances)
-
Glucose level: In patients with diabetes mellitus
-
Digoxin level: If the patient is on a digitalis medication
-
Arterial or venous blood gas: If acidosis is suspected
-
Urinalysis: To look for evidence of glomerulonephritis if signs of renal insufficiency without a known cause are present
-
Cortisol and aldosterone levels: To check for mineralocorticoid deficiency when other causes are eliminated
Electrocardiography
Electrocardiography is essential and may be instrumental in diagnosing hyperkalemia in the appropriate clinical setting. Electrocardiographic changes have a sequential progression that roughly correlates with the patient’s potassium level. Potentially life-threatening arrhythmias, however, can occur without distinct electrocardiographic changes at almost any level of hyperkalemia.
See
Workup
for more detail.
Management of hyperkalemia
Prehospital care
Prior to reaching the emergency department, treatment of a patient with hyperkalemia includes the following:
-
A patient with known hyperkalemia or a patient with renal failure with suspected hyperkalemia should have intravenous access established and should be placed on a cardiac monitor
[
4
]
-
In the presence of hypotension or marked QRS widening, intravenous bicarbonate, calcium, and insulin given together with 50% dextrose may be appropriate
-
Avoid calcium if digoxin toxicity is suspected; magnesium sulfate (2 g over 5 min) may be used alternatively in the face of digoxin-toxic cardiac arrhythmias
Inhospital care
Once the patient reaches the emergency department, assessment and treatment include the following:
-
Continuous ECG monitoring with frequent vital sign checks - When hyperkalemia is suspected or when laboratory values indicative of hyperkalemia are received
-
Assessment of the ABCs and prompt evaluation of the patient's cardiac status with an electrocardiogram (ECG)
-
Discontinuation of any potassium-sparing drugs or dietary potassium
If the hyperkalemia is known to be severe (potassium >7.0 mEq/L) or if the patient is symptomatic, begin treatment before diagnostic investigation of the underlying cause. Individualize treatment based upon the patient's presentation, potassium level, and ECG.
Dialysis is the definitive therapy in patients with renal failure or in whom pharmacologic therapy is not sufficient. Any patient with significantly elevated potassium levels should undergo dialysis, as pharmacologic therapy alone is not likely to adequately bring down the potassium levels in a timely fashion.
Medications
Drugs used in the treatment of hyperkalemia include the following:
-
Calcium (either gluconate or chloride) - Reduces the risk of ventricular fibrillation caused by hyperkalemia
-
Insulin administered with glucose - Facilitates the uptake of glucose into the cell, which results in an intracellular shift of potassium
-
Alkalinizing agents - Increases the pH, which results in a temporary potassium shift from the extracellular to the intracellular environment; these agents enhance the effectiveness of insulin in patients with acidemia
-
Beta2-adrenergic agonists - Promote cellular reuptake of potassium
-
Diuretics - Cause potassium loss through the kidney
-
Binding resins - Promote the exchange of potassium for sodium in the gastrointestinal (GI) system
-
Magnesium sulfate - Has been successfully used to treat acute overdose of slow-release oral potassium
-
Potassium binders - Bind and remove potassium from the GI tract
See
Treatment
and
Medication
for more detail.